Table of Contents
In 2019, 39.0% of U.S. adults reported back pain in the past 3 months. Back pain can force a decision fast. Most back pain is not dangerous, but a few symptoms mean you should not wait.
So, how to tell if back pain is serious? Check red flags first. New bladder or bowel changes, saddle numbness, fever, major trauma, or weakness that is getting worse should be treated as urgent. If none are present, a short trial of back pain relief and simple care steps is often reasonable.
What Makes Back Pain Serious?
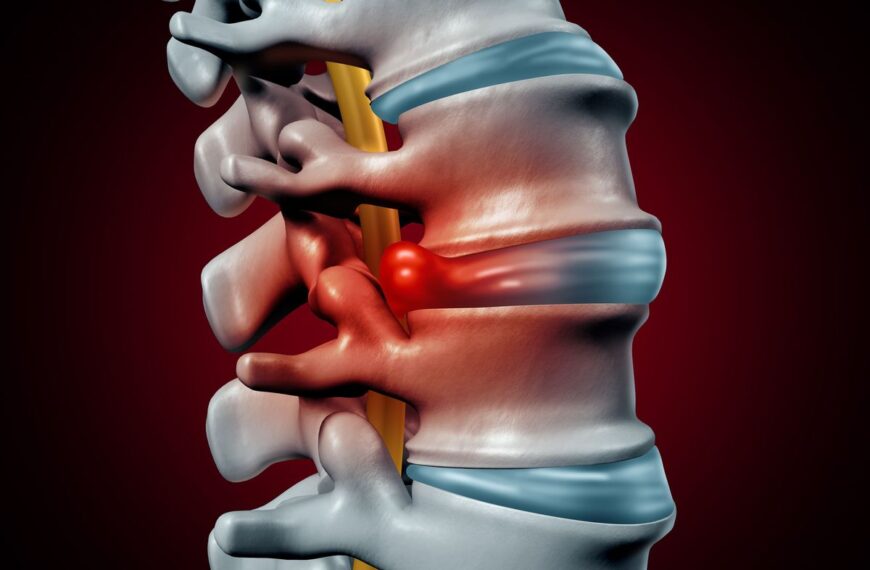
“Serious” back pain refers to symptoms that may indicate a higher-risk underlying condition requiring specific medical intervention. This includes issues like significant nerve compression (e.g., cauda equina syndrome), fracture, infection, or systemic disease.
It is critical to understand that the intensity of pain is not a reliable indicator of seriousness. A severe muscle spasm can be excruciating but not dangerous, while subtle, progressive numbness could be a critical warning sign. The type and pattern of symptoms matter most.
To provide context, while back pain is exceedingly common, the annual incidence of serious specific causes in the community is relatively low. Population studies have reported rates such as:
Vertebral fracture: ~13 per 100,000 person-years.
Spinal malignancy: ~8.5 per 100,000 person-years.
Cauda equina compression: ~4.4 per 100,000 person-years.
This data underscores a key point: while the overall risk is low, the consequences of missing a serious condition can be high. Therefore, recognizing the warning signs—detailed in the next section—is essential for making smart decisions about your care.
Which Back Pain Red Flags Mean You Should Not Wait?
These “red flags” are your body’s urgent alarms. If you experience any of the following, seek prompt medical evaluation:
A major red flag requiring immediate emergency care.
New loss of sensation in the groin, inner thighs, or buttocks.
Increasing weakness in your legs, foot drop, or sudden difficulty walking.
Fever accompanied by back pain can indicate a spinal infection.
Pain following a car accident, fall from height, or other significant impact.
New, persistent pain in this context needs investigation.
Can You Use a Two-Minute Triage Flow Right Now?
Use this simple flowchart to decide your next step:
Seek Emergency Care Now: If you have any of the red flags listed above (especially bladder/bowel changes or saddle numbness).
Schedule a Professional Evaluation This Week: If pain is severe, prevents sleep or walking, follows an accident, or isn’t improving after a few days.
Consider a Short Trial of Home Care: If you have none of the red flags, can move reasonably well, and feel slight daily improvement.
When Is It Ok to Try Home Care First?

If your self-check reveals no red flags, and you are still able to move and walk, a short, monitored period of home care is a reasonable first step. Many back pain episodes improve significantly with time and careful self-management.
Research supports this approach. A systematic review on acute low back pain shows that many people experience rapid early improvement, with mean pain and disability scores improving by about 58% within the first month.
A practical, evidence-informed timeline for a home care trial looks like this:
Day 1 to Day 3: Prioritize gentle movement over bed rest. Use ice for sharp pain or heat for stiffness. Frequently check for any red flags.
Day 4 to Day 7: Focus on a gradual return to light daily routines. The key is to note whether your symptoms show a daily trend of getting slightly better, not necessarily perfect.
Week 2: If you see no functional improvement—meaning your ability to walk, sleep, or perform basic tasks isn’t getting easier—it is time to plan a professional evaluation.
Week 6: Persistent pain that hasn’t resolved with appropriate care warrants a clinical assessment to identify the underlying cause and prevent it from becoming chronic.
The most important indicator is your functional trend. Pay closer attention to improvements in walking tolerance, sleep quality, and ease of daily tasks than to the pain score alone. If your function is declining or plateauing, that is a clear sign to seek professional guidance.
When Does Lower Back Pain Treatment Need Imaging or Lab Tests?
A common question is whether you need an X-ray or MRI right away. The guiding principle in modern care is that imaging is a tool to answer specific clinical questions, not a routine first step.
At our clinic, we follow established medical guidelines, including those from the American College of Physicians, which advise reserving diagnostic imaging for patients with higher-risk features or when serious conditions are suspected.
What Patterns Point To Common Causes Like Strain Or Sciatica?
Most back pain stems from common, mechanical issues. Recognizing patterns can help understand your pain:
Muscle Strain: Pain after lifting or twisting, often feeling like a tight ache that improves with movement.
Disc-Related Issues: Pain that may radiate, often felt worse with sitting and better with walking or changing positions.
Sciatica/Nerve Irritation: Sharp, burning, or tingling pain that radiates down one leg, often following a specific path.
What Happens in a Proper Back Pain Evaluation?

A professional evaluation is designed for clarity. At Makda Chiropractic Health Center, it includes:
A detailed discussion of your history, symptoms, and goals.
A physical and neurological exam to assess strength, reflexes, sensation, and movement.
A determination of whether imaging is needed.
A clear explanation of findings and a personalized treatment plan focused on the root cause.
Which Back Pain Relief Steps Are Reasonable While You Wait?
While arranging care, you can:
Stay mobile with gentle, frequent walks.
Use ice (for acute, sharp pain) or heat (for stiffness) for 15-20 minute intervals.
Modify activities to avoid movements that significantly worsen pain.
Try supportive sleeping positions, often on your side with a pillow between your knees.
These align with broader public health principles, such as the cdc clinical recommendations, which emphasize maximizing nonpharmacologic and nonopioid therapies for pain management.
FAQs
Note when the pain started, what makes it better or worse, and any symptoms in your legs (numbness, weakness). Also, list your main functional limits (e.g., “can’t sit for more than 10 minutes”) and relevant history, like recent accidents.
This often indicates pressure changes within the spine, possibly related to a disc. While common, if coughing causes sharp, shooting pain or new weakness, it should be evaluated.
Yes. Conditions like fractures or infections may not cause radiating leg pain. Pay attention to systemic signs like fever, unexplained weight loss, or unrelenting pain.
Aim for improved function, not necessarily being pain-free. Success is being able to walk a bit further, sleep more comfortably, or perform daily tasks with greater ease.
Intermittent pain can still be serious. A concerning pattern is pain unrelated to movement that worsens over time or consistently disrupts sleep. Tracking the overall trend is key.
Any back pain after an auto injury should be evaluated. We specialize in these trauma cases and look for issues like whiplash or disc injury that may not be immediately apparent.
New or worsening weakness (e.g., foot slapping, knee buckling) is a significant red flag for nerve involvement and needs timely assessment.
Numbness alone can signal nerve irritation. Note its location and stability. Sudden numbness in the saddle area or progressive numbness are urgent signs.
Key Takeaways
Red flags (like neurological changes or trauma) matter more than pain intensity.
Monitor your functional trend—improvement is a positive sign.
Professional evaluation provides a clear diagnosis and a structured path to recovery.
Specialized assessment is crucial for pain following events like car accidents.
If you’re questioning the severity of your back pain, you deserve a clear answer. Don’t guess. A professional evaluation can provide the clarity and direction you need. We combine over 25 years of specialized experience with a focused assessment to determine if your pain is a simple strain or something requiring specific care.
Take the next step toward understanding your back pain. Schedule a professional evaluation with us today.
📞 Call (703) 933-3838 🌐 Book Online: makdachiropractic.com